An event intended to educate prevention advocates about cannabis covered recent WAPC call data, modes of use, youth usage, and ways to communicate prevention messaging to young people.
Here are some observations from the Wednesday December 9th Washington Poison Center (WAPC) webinar “Let’s Talk Cannabis: A capacity building training for influential adults.”
My top 3 takeaways:
- WAPC Public Health Education and Communication Specialist Alex Sirotzki led the presentation which offered insight on “Exposure Trends During the COVID-19 Pandemic” and mentioned a rise in polydrug use associated with fatal car crashes (audio - 15m).
- The WAPC presentation dealt with many cannabis topics that the Northwest Prevention Technology Transfer Center (NW PTTC) webinar on cannabis pharmacology covered on October 29th.
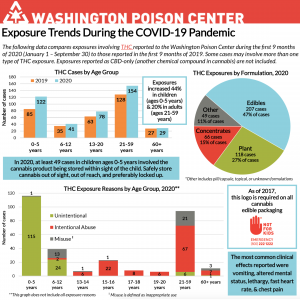
- WAPC staff prepared data “comparing the first nine months of 2019 to the first nine months of 2020” as the coronavirus pandemic impacted life across the state. Sirotzki discussed the information while reviewing the acute effects of cannabis, calling it a “pretty new...snapshot” of calls WAPC received which showed an “increase in all age categories here over time, this is continuing a trend we’ve noticed for a while.”
- He identified the “two largest age groups here would be zero to five years of age, and 21 to 59 years of age” noting that almost every case from persons five or younger was “unintentional, that just means an accident, a kid...got into an edible or something.”
- For older consumers, Sirotzki explained that WAPC found most calls were “intentional abuse” from individuals attempting to “seek intoxication.”
- As with prior years, “most calls to us in 2020 were edibles...a little over a quarter were for plant material, about 15% were concentrates” along with 49 cases for “other” cannabis items, Sirotzki said.
- He reasoned that the Not For Kids logo with WAPC’s phone number, a requirement for cannabis edibles and infused beverages, “could account for why we get so many calls on edibles.” He surmised that if the logo were on all of Washington’s legal cannabis products, “I’d wager we’d see higher case calls for these other types.”
- While reviewing 2018 data from the Washington Traffic Safety Commission (WTSC), Sirotzki observed that State officials had found “an increase in what we call polysubstance [driving under the influence] DUIs” when “using more than one substance at a time.” He noted that “the most commonly combined substance[s]...are alcohol and [tetrahydrocannabinol] THC, we see that going up quite a bit since about 2011” in fatal car collision statistics. Sirotzki said that “combining cannabis and alcohol actually increases impairment and motor vehicle crash risk more than either substance alone.”
- The U.S. Centers for Disease Control and Prevention (CDC) advises that “using alcohol and marijuana at the same time is likely to result in greater impairment than when using either one alone.” The CDC’s Morbidity and Mortality Weekly Report (MMWR) shared research on polysubstance DUIs which stated “Research has determined that co-use of marijuana or illicit drugs with alcohol increases the risk for driving impairment” citing studies from the National Institute on Drug Abuse (NIDA) and research in Italy.
- Sirotzki’s presentation covered current and emerging trends in the modes of cannabis use (audio - 22m).
- Looking at Modes of Use, Sirotzki remarked that there were “many ways that a given substance can get into the body” and cannabis had “quite a few rather common and some less common ways.” These methods could pose “unique health considerations,” narrow choice to particular cannabinoid profiles, and lead to “really weird” differences in measuring dosage, he indicated. Flowers and concentrates typically used a percentage of THC, while infused products and tinctures used a cannabinoid “volume” measurement, Sirotzki explained. He felt that a “cultural understanding” existed around the relative strength of beer or wine compared with liquor but “because cannabis is such a new product, in the legality” a similar understanding for the relative strength of cannabis products “isn’t widespread.”
- Smoking. Sirotzki said the simple method of breathing in combusted cannabis flower from a joint, pipe, or bong was “a common approach.”
- Edibles and Infused Beverages. “There’s a lot to say about edibles,” he told the group. Sirotzki felt a diversity in “serving size” containing between 1 and 10 milligrams of THC could be confusing for consumers. He was also concerned about the “delay in onset of effects,” particularly when considering driving as it was possible an edible might “kick in” later when an individual was behind the wheel, in addition to the fact that “the intoxication from edibles can last a lot longer than other methods.”
- Vaping. Sirotzki believed the term “vaping” was misleading as it “implies that it's just water vapor” when in fact vape devices create “an aerosol” of very small cannabis “oil particles.” He added that vapor devices could utilize “solid concentrates” as well as “liquid concentrates” both of which had higher percentages of THC than found in flowers. Sirotzki suggested those with an interest in the method attend WAPC’s “Finding the Truth Among the Vapors” webinar on December 16th.
- Dabbing. “Some folks will say that the term dabbing and the term vaping really are interchangeable,” he argued, while others deem it “similar to vaping” while using “much, much, much higher heat.” Sirotzki focused on “high heat” dabbing, saying the setup looked “kind of like a bong” with aerosol cooled by the water prior to inhalation. The difference, he said, was using concentrates with a high THC percentage on “superheated metal...or quartz” to vaporize the substance for inhalation. The use of blowtorches created a “potential for burns,” Sirotzki commented, along with a “high dose” which impacts consumers “very, very rapidly.”
- Asked in chat how the method was related to the dance move dabbing, he said he’d “heard so many versions” around the level of association between uses of the term but no “analysis or documentary” sufficiently proved or debunked the connection.
- Sirotzki called attention to the Nectar Collector which he’d learned about from “a very excited” retail budtender who said “for that shop it was becoming pretty popular” and was “essentially a straw” with a heated tip that could vaporize from “a pool of concentrated” butane hash oil (BHO).
- Alternative methods. Other methods were coming out “all the time,” Sirotzki reported, including oil-based tinctures that “bring on effects faster than an edible,” in addition to topical products and “apparently, suppositories.”
- Sirotzki polled the audience regarding “the most common methods you know of from youth in your life.” Responses indicated that “folks are hearing more about vaping” as well as smoked cannabis. He mentioned the State’s latest Healthy Youth Survey (HYS) published in 2019 showed “more kids were reporting that they smoked it, rather than these other methods.” Sirotzki conveyed his understanding that the survey, delayed by COVID-19, would next be collected in 2021.
- Washington State Liquor and Cannabis Board (WSLCB) Public Health Education Liaison Sara Cooley Broschart discussed the 2018 HYS at length with board members on January 8th.
- Looking at Modes of Use, Sirotzki remarked that there were “many ways that a given substance can get into the body” and cannabis had “quite a few rather common and some less common ways.” These methods could pose “unique health considerations,” narrow choice to particular cannabinoid profiles, and lead to “really weird” differences in measuring dosage, he indicated. Flowers and concentrates typically used a percentage of THC, while infused products and tinctures used a cannabinoid “volume” measurement, Sirotzki explained. He felt that a “cultural understanding” existed around the relative strength of beer or wine compared with liquor but “because cannabis is such a new product, in the legality” a similar understanding for the relative strength of cannabis products “isn’t widespread.”
- The presentation explored why school-age youth reported using cannabis and suggested strategies for communicating prevention messages to them.
- Why Youth Use (audio - 11m). Sirotzki opened this portion of the event by asking attendees to share their responses to the question of why youth use cannabis in the webinar chat box. He recited responses such as “everyone does it,” “because it is funny,” “helps with anxiety,” and in order to “sleep better.”
- He then cited research by the King County Youth Marijuana Prevention and Education Program (KC YMPEP) which conducted 26 listening sessions to collect 202 youth participant responses which outlined reasons for cannabis use including:
- Peer pressure
- Curiosity
- Sense that “everyone else is doing it”
- To cope with stress (self-medicate)
- The sessions also identified popular reasons youth gave for not using cannabis, which Sirotzki termed “protective factors”:
- Fear of consequences (re: school, activities, and future goals)
- Support from peers and family
- Knowledge of health risks
- Sirotzki explained that respondents indicated that “popularity was actually more influential than awareness of the possible risks” and that “cannabis use feels more normalized since legalization.” Additionally, he said the medical uses of cannabis “sort of separates it out from other substances.”
- Next, Sirotzki talked about “physiological dependence” or “when the body/brain begins to rely on an external substance to maintain normal function.” He admitted he was likely dependent on caffeine, having developed a high tolerance and withdrawal symptoms like lethargy, sleepiness, and headaches. “Addiction is when physical dependence starts to become disruptive to other aspects of life,” he said. Cannabis was “not as addictive as heroin or nicotine,” Sirotzki reported, but “very few things'' were that addictive. He claimed “regular cannabis users who quit often report that they experience withdrawal symptoms” which “implies dependence.” But Sirotzki cautioned that some signs of withdrawal “may actually overlap with reasons why someone might use cannabis in the first place.”
- The National Academies of Sciences, Engineering, and Medicine (NASEM) had defined Problem Cannabis Use as that which “includes the experience of persistent or recurrent social, interpersonal, occupational, academic, recreational, psychological, or physical problems caused or exacerbated by cannabis use.” Under such a definition, Sirotzki stated, risk factors for problem use included “initiating cannabis at an early age and being male, alongside with smoking cigarettes.” Moreover, “we very likely know of a correlation” between being male, increased “frequency of use,” and “the severity of problem cannabis use,” he observed. Sirotzki remarked that there was less evidence supporting other suspected adolescent risk factors such as “major depressive disorder...parental substance use, poor school performance,” or other Adverse Childhood Experiences (ACEs) “which can be risk factors for a great number of things.”
- Sirotzki mentioned that the “gateway hypothesis” for cannabis use as a precursor to wider substance use problems was “really tricky with cannabis.” He said for adults, “we probably know that cannabis use is correlated with substance use disorder for alcohol, tobacco, and other illicit substances.” However, Sirotzki explained that this was not the same as cannabis causing the other disorders, many of which could be correlated to the same risk factors. Sirotzki suggested that health experts “may know that cannabis use is correlated with tobacco use initiation” but there was “actually more evidence for the other direction, that starting tobacco may increase the likelihood that someone starts using cannabis.” He said these same correlations had also been observed around youth cannabis use.
- Treatment for cannabis use disorder “seems to be very effective,” Sirotzki commented, and the methods had been used “in a lot of other substance use disorder treatment.” The common forms of treatment included:
- Communication: What do youth want? (audio - 4m). Sirotzki briefly went through communication strategies which emerged during the King County listening sessions when “facilitators asked youth ‘What do you want to know?’ and, like, ‘how do you want to know it?’”
- Participants reported wanting “unbiased information on the health effects” and “how cannabis works as well as research on its risks and benefits. And they really did not like exaggeration or shaming or scare tactics.” Sirotzki inferred that youth were “suspicious” of bias or agendas from both health experts and the cannabis industry, instead preferring “relevant risk messaging” in an “open discussion with accurate information with folks they trust.” This was a process that “acknowledged the agency of youth,” he said, as well as their “decision making ability.”
- Sirotzki told attendees that participants also voiced a need for “messaging placed where youth already engage” like social media, but also identified “magazines which was kind of surprising, I didn’t think youth looked at magazines all that much anymore.”
Information Set
-
Announcement [ Info ]
-
Registration [ Info ]
-
Presentation [ Info ]
-
Complete Audio - Cannabis Observer
[ InfoSet ]
-
Audio - Cannabis Observer - 00 - Complete (2h 20m 26s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 01 - Welcome - Alex Sirotzki (5m 24s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 02 - WAPC Background - Alex Sirotzki (3m 44s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 03 - How Cannabis Works - Alex Sirotzki (7m 12s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 04 - Legality and History - Alex Sirotzki (10m 25s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 05 - Adult-Use and Medical Cannabis - Alex Sirotzki (7m 21s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 06 - Breakout Sessions - Alex Sirotzki (2m 12s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 07 - Breakout Session - Group D (7m 45s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 08 - Breakout Sessions - Follow Up - Alex Sirotzki (2m 42s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 09 - Modes of Use - Alex Sirotzki (21m 58s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 10 - Labeling - Alex Sirotzki (5m 58s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 11 - Acute Effects - Alex Sirotzki (15m 11s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 12 - Break (43s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 13 - Why Youth Use Cannabis - Alex Sirotzki (10m 58s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 14 - Cannabis Trends - Alex Sirotzki (12m 11s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 15 - Health Risks - Alex Sirotzki (9m 22s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 16 - Communicating with Youth - Alex Sirotzki (3m 40s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 17 - Breakout Sessions - Alex Sirotzki (5m 39s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 18 - Advocacy and Resources - Alex Sirotzki (2m 14s; Dec 14, 2020) [ Info ]
-
Audio - Cannabis Observer - 19 - Wrapping Up - Alex Sirotzki (5m 50s; Dec 14, 2020) [ Info ]
-
-
WAPC - Webinar - General Information
[ InfoSet ]
- No information available at this time